ED process improvement consulting and interim leadership helps implement a middle- trac process, improving flow
Philips provided an Interim ED Manager, Interim ED Director, and led an intensive multidisciplinary Performance Improvement Consulting initiative which identified several opportunities to increase process efficiency and patient flow.
The ED at St. Mary Medical Center (SMMC) in Apple Valley, CA was challenged with significant volume growth, recurring gaps in ED leadership, prolonged lengths of stay, and high LWBS rates. SMMC asked Philips to provide interim ED leadership and performance improvement in the ED.



An innovative approach to ED performance improvement
Strong interim leadership Philips consultants joined SMMC as Interim ED Manager and ED Director, focused on day-to-day operational and staff management. Leadership responsibilities included staff communications/relationships/support, hiring vacant staff positions and resource planning, staff development and training, assisting with conflict resolution, team mentoring, and more. They quickly became valuable leaders of the team. A comprehensive assessment of key operational metrics was completed and a performance improvement (PI) engagement was recommended. Adding the PI program allowed the interim leaders to focus on team management while supporting the operational efficiency process changes. A third consultant joined to focus on leading teams towards improving key performance indicators. The third consultant supported SMMC during these improvement initiatives and the two other consultants were asked to continue in the interim roles for the long-term.
ED Performance Improvement Several areas were identified as needing improvement, including actions to: A PI work team was organized, led by Philips consultants and included SMMC physicians, administrative leaders, ED staff, and ancillary staff. The task was to collaboratively agree to an action plan to improve the ED walkout and length of stay rates. The work team completed a deep dive review into each area identified in the assessment and leveraged the data analysis and stakeholder input gathered earlier. They developed recommendations for process change, prioritizing change initiatives which could make the greatest impact.
The performance assessment included a thorough analysis of data collected for volume, arrival patterns, staffing patterns, ESI level distribution, ED billing visit level distribution, disposition breakdown, and length of stay. The consultants conducted interviews with administrators, departmental leaders, and staff, and spent considerable time observing ED patient flow, staff workflow, departmental processes, and communication.
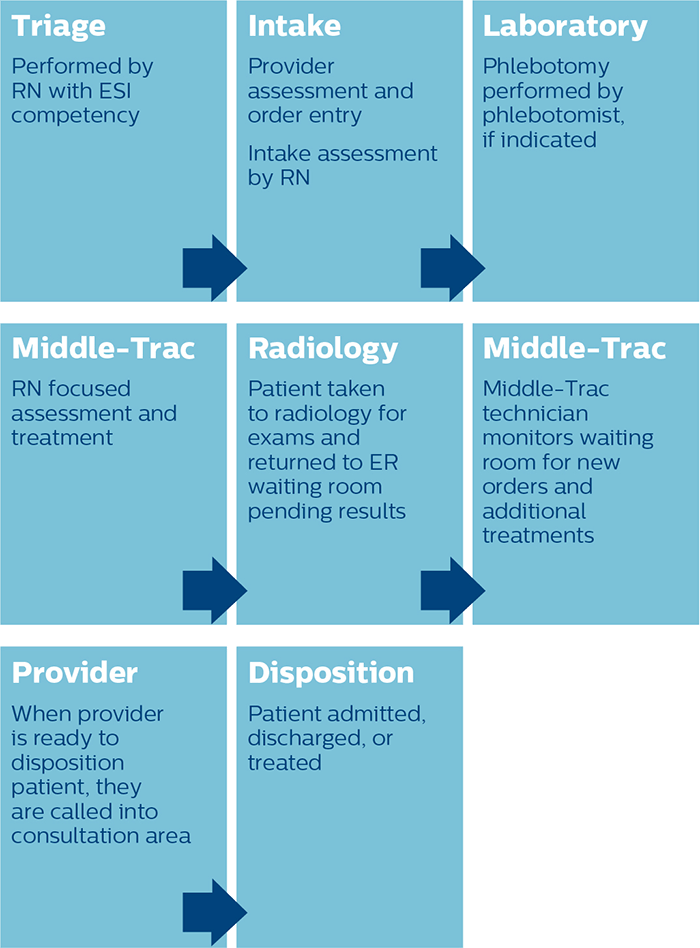
Middle-Trac patient flow process Similar to an assembly-line, elements of the Middle-Trac process work cohesively. A triage nurse classifies arriving patients into one of three categories: immediate bed needed, fast track appropriate, and remaining Middle-Trac patient population. A detailed process flow maximizes continuity of care, manages essential resources, and minimizes provider hand-offs.
Key to supporting the PI recommendations was development of a new process solution termed ‘Middle-Trac’. Derivative of a split-flow process where patients are triaged quickly into parallel care streams, Middle-Trac focuses on patients in the middle (ESI level 3) who do not require immediate treatment. It keeps these patients vertical and moving through the department, not occupying valuable treatment spaces until a disposition decision is made.
SMMC Middle-Trac process flow
"The Philips consultants provided exceptional leadership and became part of our team. They helped identify, develop, and implement process change which has had a significant impact on our patient throughput as well as patient and staff satisfaction."
Marilyn Drone, MSN, RN
Executive Vice President, Chief Operating Officer, and Chief Nursing Officer, St. Mary Medical Center
Results*
The Philips-SMMC team was successful in implementing process changes that significantly improved door-to-provider times, ED length of stay, and the left without being seen rate for Middle-Trac patients. Two Philips consultants were asked to remain in the interim leadership roles long-term.
As a result of the engagement, SMMC was able to achieve the below results*:



* Results from case studies are not predictive of results in other cases. Results in other cases may vary.

Meet our team

Dan Hannan, MBA, BSN, BS, RN Senior Consultant
Dan brings 30+ years of clinical care and leadership experience focused on ED and hospital-wide operations, informatics, throughput, and patient experience. He has helped providers reduce left without being seen, arrival-to-room, and ED length of stay.
You are about to visit a Philips global content page
Continue
JoAnn Lazarus, MSN, RN, CEN, FAEN Principal and Practice Operations Lead, Retired
JoAnn was a leader for the emergency services team, providing interim leadership and leading process improvement projects. Among her accomplishments include establishing a fast track, a middle track, implementing a SWAT team for the waiting room, and decreasing the walk out rate by 25% in a 100,000-visit level 1 academic trauma center.
You are about to visit a Philips global content page
ContinueCustomer story
-
![87% reduction in ED arrival-to-room at FirstHealth Moore]()
-
![87.5% reduced ED arrival-to-triage at McLeod Health Clarendon]()
Customer story
87.5% reduced ED arrival-to-triage at McLeod Health Clarendon
Click here to learn more