Filter by area:
- Customer story
![Creating an engaging X-ray environment]()
Creating an engaging X-ray environment
Ambient Experience solutions help Children’s of Alabama create a calming X-ray room environment for patients and staff.
Click here to learn more - Webinar
![Smart hospitals - the four guiding principles]()
Smart hospitals - the four guiding principles
Edgar van Zoelen and Angus Cameron provide their insights on how smart hospitals can play a pivotal role in the smart and connected healthcare system of the future.
Click here to learn more - Customer story
![Creating a roadmap for sustainable hospital operations]()
Creating a roadmap for sustainable hospital operations
Learn how Philips performed a detailed analysis to help Gemeinschaftskrankenhaus Havelhöhe develop a sustainability roadmap.
Click here to learn more - Customer story
![Helping to design and plan for a state-of-the-art cardiology institute]()
Helping to design and plan for a state-of-the-art cardiology institute
Our consultants helped optimize the footprint, increase clinical workflow efficiency, and enhance the care experience for both patients and staff of the planned facilities.
Click here to learn more - Article
![Testing resilience strategies in a digital twin]()
Testing resilience strategies in a digital twin
Sudin Kansakar shares his insights on how digital twin capability can help manage winter capacity.
Click here to learn more - White paper
![Strategies to improve patient experience in cath lab procedures]()
Strategies to improve patient experience in cath lab procedures
This research paper provides a retrospective review in validation of patient-focused design concepts, and concludes that patients are looking for enhancements both outside of and within the cath lab.
Click here to learn more - Customer story
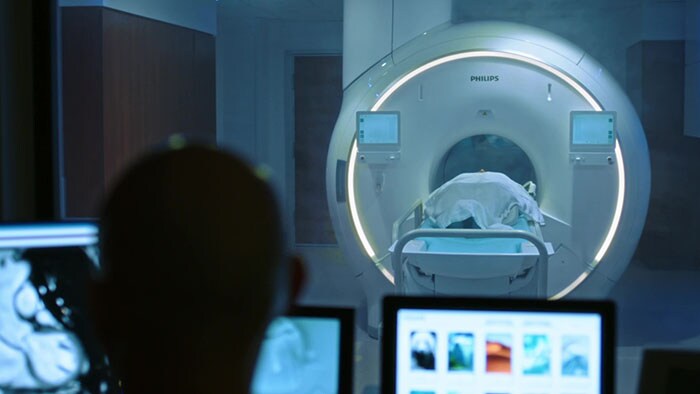
![Relaxing MRI environment - Chiba University Hospital]()
Relaxing MRI environment - Chiba University Hospital
Discover how Chiba University Hospital teamed up with the Philips Ambient Experience team to deliver a dynamic lighting, projection, and sound solutions to help provide a calming and engaging environment for patients and an efficient workplace for staff in the MRI rooms.
Click here to learn more - Article
![Key eHealth strategy learnings]()
Key eHealth strategy learnings
Egil Nilsen shares his insights on how the pandemic fast-tracked healthcare digital transformation, in this article on Key eHealth strategy learnings from the pandemic.
Click here to learn more - Webinar
![Best practices in how to reduce alarm fatigue]()
Best practices in how to reduce alarm fatigue
A team approach to improving the acoustical environment
Click here to learn more - Customer story
![Concept design and floor plan of the future cath lab department]()
Concept design and floor plan of the future cath lab department
Amsterdam UMC will combine two cath lab departments into a single location. Philips consultants helped translate their vision for better heart care into a concept design, floor plan and a 3D animation of their new cath lab department.
Click here to learn more - Article
![The strategic role of ASCs in cardiology care]()
The strategic role of ASCs in cardiology care
Deb Thompson and Chris Comeau share insights on the migration of cardiovascular procedures to ASCs
Click here to learn more - Customer story
![Improving imaging workflow efficiencies]()
Improving imaging workflow efficiencies
Radiology workflow improvements to provide efficient quality of care
Click here to learn more - Customer story
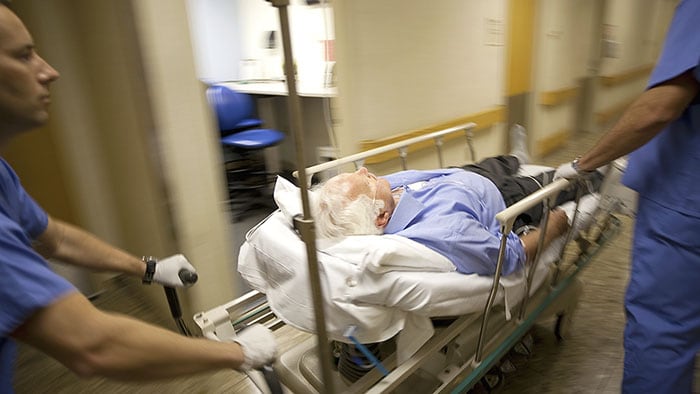
![22% increase in direct bedding]()
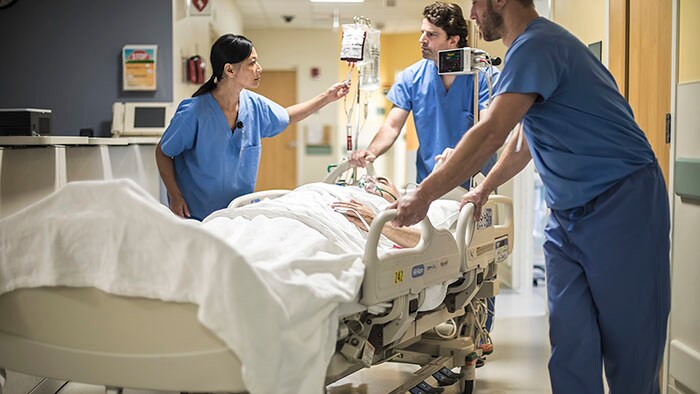
22% increase in direct bedding
Adrz hospital engaged Philips consultants to help develop new processes and work agreements in their emergency department to cope with peak volumes, resulting in 22% increase in direct bedding, 21% decrease in patient waiting time and a 5 min reduction in turnaround time per patient.
Click here to learn more - Customer story
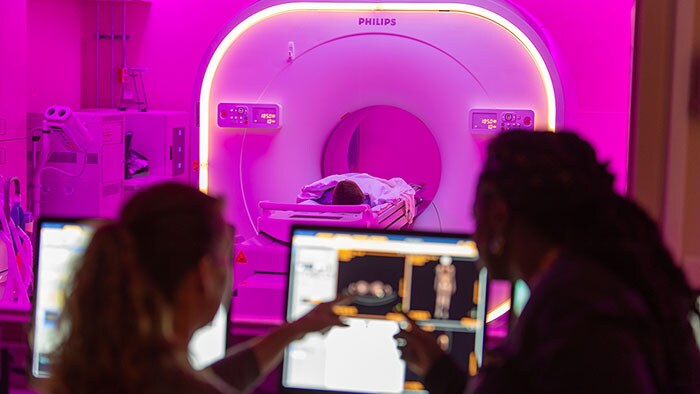
![Phoenix Children’s Hospital finds efficiency and calm in pediatric imaging]()
Phoenix Children’s Hospital finds efficiency and calm in pediatric imaging
Ambient Experience and the Vereos Digital PET/CT help achieve exceptional images while reducing radiation dose.
Click here to learn more - Customer story
![Miami Cardiac & Vascular Institute puts people at the heart of diagnostic procedures]()
Miami Cardiac & Vascular Institute puts people at the heart of diagnostic procedures
Miami Cardiac & Vascular Institute uses Philips Ambient Experience to help a COVID-19 patient through a cardiac MRI
Click here to learn more - Article
![Strategies for combating nurse burnout during and after the pandemic]()
Strategies for combating nurse burnout during and after the pandemic
Renee Cecil shares her insights on nurse burnout, the effects of the pandemic on nurses, and how nurse leaders can reduce burnout.
Click here to learn more - Customer story
![Optimizing workflow efficiency to improve throughput and enhance the patient experience at WellSpan York Hospital]()
Optimizing workflow efficiency to improve throughput and enhance the patient experience at WellSpan York Hospital
Clinical consultants assessed processes and helped implement effective change for improved patient throughput and $1.7m cost savings over 3 months
Click here to learn more - White paper
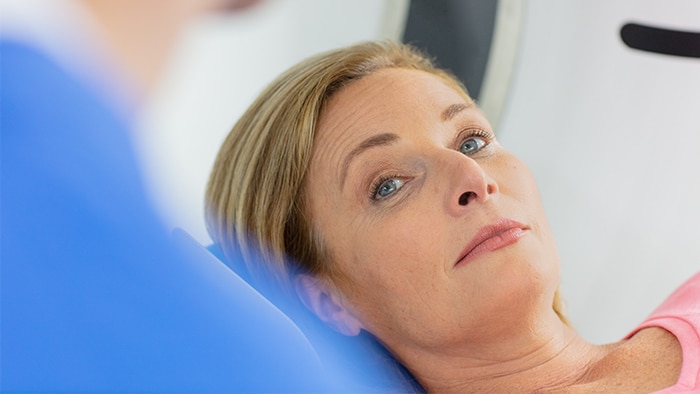
![The cost of fear and anxiety in radiology]()
The cost of fear and anxiety in radiology
Philips provides the latest insights into how you can reduce negative feelings and their impact on your radiology examinations and operations.
Click here to learn more - Article
![Emergency Severity Index, is it broken?]()
Emergency Severity Index, is it broken?
Brian Armstrong and Renee Cecil share insights on the strengthening the use of ESI to improve patient care
Click here to learn more - Video
![Evaluating telemetry monitoring and alarm management processes at Huntsville Hospital]()
Evaluating telemetry monitoring and alarm management processes at Huntsville Hospital
John Davanzo, Dale Roberts and Wendy Cantrell partner to improve telemetry monitoring and alarm management processes
Click here to learn more - Article
![Emergency preparedness – not an ‘if’ but a ‘when’]()
Emergency preparedness – not an ‘if’ but a ‘when’
John Davanzo shares lessons learned on emergency preparedness from COVID-19 and preparing for the future
Click here to learn more - Customer story
![Optimizing a telemetry monitoring program at Huntsville Hospital]()
Optimizing a telemetry monitoring program at Huntsville Hospital
Clinical consultants identify various opportunities to improve telemetry and alarm management processes.
Click here to learn more - Customer story
![77% reduced downtime in the central OR]()
77% reduced downtime in the central OR
Philips helped Universitätsklinikum Hamburg-Eppendorf optimize its OR capacity and increase staff satisfaction resulting in 1400 more surgeries, 77% reduced downtime in the central OR and improved staff satisfaction.
Click here to learn more - Article
![Insights on how to improve emergency preparedness]()
Insights on how to improve emergency preparedness
Brian Armstrong was interviewed by HealthLeaders to share his insights on emergency preparedness and preparing for the future.
Click here to learn more - Webinar
![Enhancing the pediatric radiology environment]()
Enhancing the pediatric radiology environment
Imaging experts from Phoenix Children's Hospital share their experience with the digital PET/CT scanner and Ambient Experience.
Click here to learn more - White paper
![5 best practices for optimized imaging services]()
5 best practices for optimized imaging services
Mel Allen explains how optimized imaging services can further support the Quadruple Aim.
Click here to learn more - Customer story
![Helping to create an alarm management roadmap]()
Helping to create an alarm management roadmap
Delivering alarm management performance improvement expertise to reduce non-actionable alarms
Click here to learn more - White paper
![Strategies to optimize telemetry utilization]()
Strategies to optimize telemetry utilization
Performance improvement strategies for improve telemetry utilization for decreased LOS and increased capacity
Click here to learn more - Webinar
![Collaborating to improve surgical services performance at Nash UNC]()
Collaborating to improve surgical services performance at Nash UNC
Discover how Peggy Clifton and Julie Lawler collaborated to positively impact patient throughput across the surgical continuum
Click here to learn more - Customer story
![Streamlining patient placement to support improved throughput]()
Streamlining patient placement to support improved throughput
Performance improvement consulting implements capacity management improvements in bed assignment and workflow
Click here to learn more - Article
![Bridging the generational divide]()
Bridging the generational divide
Lisa Manion, MD shares her insights on leveraging the strengths and value of providers at all ages.
Click here to learn more - Customer story
![57% decrease of admission freezes for Chest Pain Center]()
57% decrease of admission freezes for Chest Pain Center
Philips helped the cardiology department at the Reinier de Graaf Hospital to improve throughput of clinical cardiology patients, resulting in a 57% decrease of admission freezes for the Chest Pain Center** and patients go home an hour earlier.
Click here to learn more - Webinar
![Becoming informed - preparing for a winter surge using trauma-informed care tactics]()
Becoming informed - preparing for a winter surge using trauma-informed care tactics
During this webinar, Philips will discuss trauma-informed care from a historical perspective and the traditional use of trauma-informed care in hospitals.
Click here to learn more - White paper
![Enhancing ED culture and process efficiency]()
Enhancing ED culture and process efficiency
Improving the culture and employee engagement to support process improvement in an emergency department
Click here to learn more - Video
![Implementing an alarm management plan at Advocate Aurora Health]()
Implementing an alarm management plan at Advocate Aurora Health
Hear how Lisa Pahl and Melinda Jamil of AAH collaborated to implement alarm changes and reduce non-actionable alarms.
Click here to learn more - Customer story
![Cultivating change in surgical services at Nash UNC Health Care]()
Cultivating change in surgical services at Nash UNC Health Care
Performance improvement consultants developed processes and strategies to enhance surgical services.
Click here to learn more - Article
![Reducing non-actionable alarms and alarm fatigue with AU Health]()
Reducing non-actionable alarms and alarm fatigue with AU Health
Lisa Pahl supported a team-based approach which helped implement effective alarm reduction interventions in an adult ICU. (gated article).
Click here to learn more - Customer story
![Design of a radiology department]()
Design of a radiology department
University Hospital in Linköping, Sweden engaged Philips to help with a strategic design project for Linkoping’s radiology department. Our consultants used a 360° assessment including a fast and cost-effective planning and redesign process, to address the clinical, and operational needs, technology innovation, and patient and staff experience.
Click here to learn more - Customer story
![Restructured ICU bed planning process]()
Restructured ICU bed planning process
Krankenhaus Düren engaged Philips to help improve their ICU bed management, by gathering insights and identifying areas for improvement to make better use of their ICU bed capacity.
Click here to learn more - Article
![How to avoid the fallout after a change in nurse leadership]()
How to avoid the fallout after a change in nurse leadership
Interim leaders help stabilize an emergency department, keep staff engaged, and keep the unit running efficiently.
Click here to learn more - Article
![Leveraging lean to drive ED efficiency]()
Leveraging lean to drive ED efficiency
Lowell Hardin shares insights on how EDs can leverage lean theories to increase efficiency in patient care.
Click here to learn more - Customer story
![Analytics dashboard helps avoid $1.3m expense at Beverly Hospital]()
Analytics dashboard helps avoid $1.3m expense at Beverly Hospital
Analytics consulting and a custom performance dashboard helped improve ED processes and avoid $1.3m in unnecessary additional staffing
Click here to learn more - Article
![Insights to minimize workplace violence]()
Insights to minimize workplace violence
Will Stewart shares his insights on how healthcare institutions and their workforce can leverage unconditional positive regard to respond to situations of violence in high stress situations.
Click here to learn more - Customer story
![Enhancing radiology experience at Children’s Omaha]()
Enhancing radiology experience at Children’s Omaha
Our design consultants helped optimize the pediatric radiology care environment, with a 10% construction cost savings.
Click here to learn more - Customer story
![Quick Scan unlocks insights for cath lab department]()
Quick Scan unlocks insights for cath lab department
Rijnstate engaged Philips to help optimize work processes, and setup for a new cardiac catheterization department. Using the Integrated Cardiovascular Solutions Quick Scan, a department-wide analysis of various quality parameters was done and clear opportunities for the short- and long-term were identified.
Click here to learn more - Article
![Key success criteria for outpatient heart failure clinics]()
Key success criteria for outpatient heart failure clinics
Deb Thompson discusses what is required for the efficient management of a multi-disciplinary heart care team.
Click here to learn more - Customer story
![Engaging staff helps improve imaging services]()
Engaging staff helps improve imaging services
Wye Valley NHS Trust engaged Philips to help improve the quality and productivity of its imaging services. Philips consultants delivered a foundational level training course to imaging staff and a focused improvement project to the MR group. The Trust expects to improve workflow and increase productivity by 5-10% per year.
Click here to learn more - Webinar
![Improving emergency department efficiency at FirstHealth Moore]()
Improving emergency department efficiency at FirstHealth Moore
Learn how Philips consultants helped create sustained improved ED operational performance and an enhanced patient experience.
Click here to learn more - Customer story
![Improved imaging workflow for volume growth at Rochester General Hospital]()
Improved imaging workflow for volume growth at Rochester General Hospital
Our consultants helped optimize operational efficiency to support volume growth and a planned imaging service line expansion.
Click here to learn more - Customer story
![Cardiac careflow optimization]()
Cardiac careflow optimization
Heart Hospital TaUH engaged the Philips consulting team to help understand gaps between processes and practices, and to define a set of cardiac careflow improvement initiatives that could be implemented in their current and new facility
Click here to learn more
*Results from case studies are not predictive of results in other cases. Results in other cases may vary.