How interoperability and cybersecurity jointly deliver the promise of connected care
We are entering a new era of opportunity in connected care. Health systems need to realize the full benefits of interoperability – and cybersecurity—to take their connected care strategy to the next level. Our end-to-end design mindset helps you create secure, seamless interoperability across multi-vendor systems as well as collaboration between multi-disciplinary teams.
Discover new opportunities in connected care
Transforming barriers into enablers. See how to connect and secure data across care settings and teams.
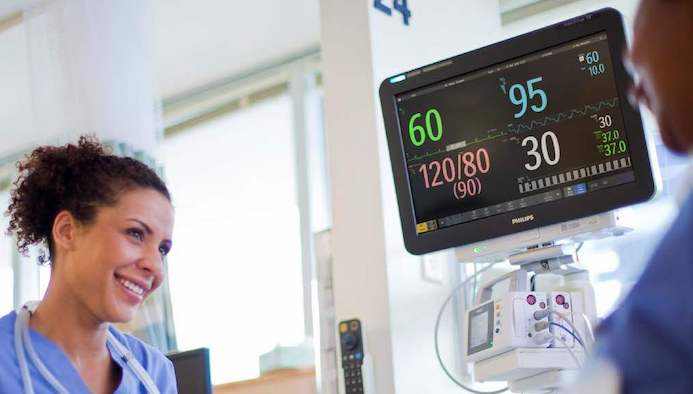
Complete the clinical picture
We link the most up-to-date patient data between care teams and multi-vendor systems, leveraging our clinical expertise and end-to-end design mindset to solve your interoperability challenges.
Read more about our interoperability solutions:
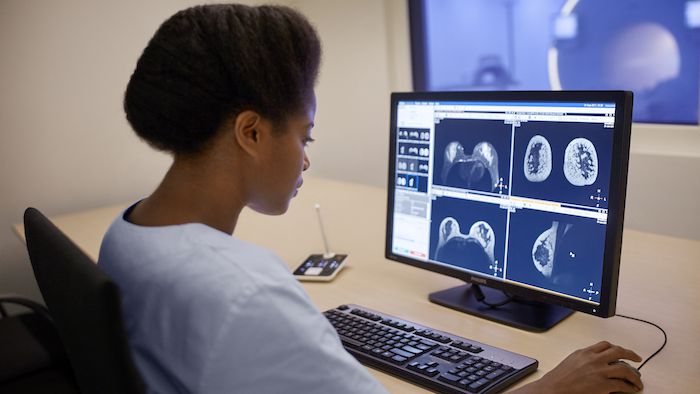
Safeguard the connections that matter most.
We take a proactive approach to protecting sensitive across devices, systems and settings.
Read more about our approach to Cybersecurity:
Connecting and securing data and systems to help improve patient care and safety
The future of connected care requires:
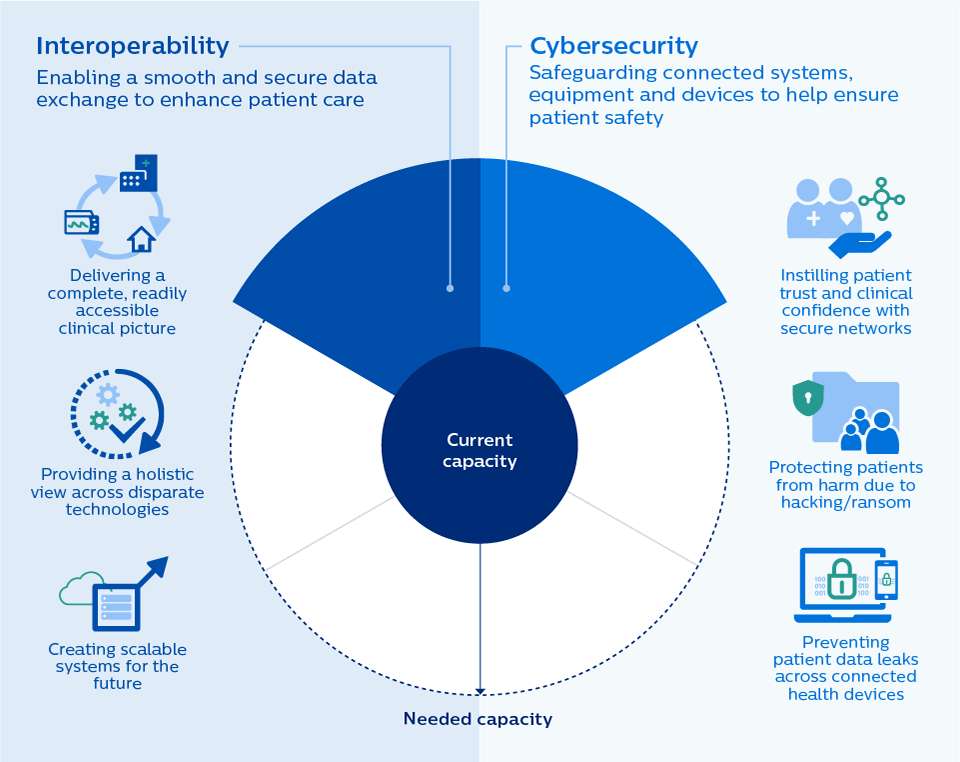
Learn how we are helping health systems create secure connections to care

The Veterans Association
See how we partnered with the VA to create virtual clinics throughout the United States allowing veterans to consult with VA providers at their local post through virtual appointments.

