Given current incentives – however unintended – it’s no surprise that clinical teams often stake claims to patient monitors and supplies that might travel outside their domains. They might label them. They might squirrel them away. Or they might do both. After all, they need to know that they can find what they need and that it will work. In a way, they’re just responding to siloed budgeting, mixed equipment types and configurations, and fragmented workflows. But such actions can also affect patient care, workloads and operations. So how best to make "culture of mine" a thing of the past?
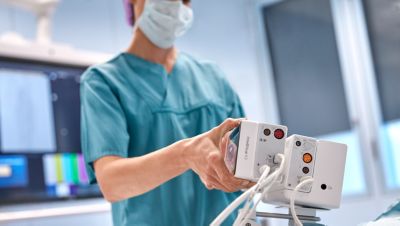
While culture of mine is a product of the environment in which many care teams operate, it comes with ongoing, negative ramifications. Spending time searching for monitors and supplies draws clinical teams away from attending to patients. Stockpiling equipment can affect availability elsewhere, potentially delaying care. And it can stand in the way of innovative, cross-unit workflows and cause teams to place unnecessary orders for additional equipment.
It's time to find a better way, one that can establish trust – trust that reliable equipment is going to be there where and when teams need it. Fortunately, health systems who have tackled the challenge have tips to share:
Within health systems, monitors and supplies often vary from hospital to hospital – and even between units within the same site. This mishmash encourages care teams to stockpile equipment, for assurance that they have monitors they can count on and compatible supplies at the ready. By standardizing with a reliable solution across the care site – and ideally the whole enterprise – health systems can encourage sharing. This standardization should extend to software revisions and monitor configurations, with flexibility in the latter for thoughtful and coordinated tailoring to care units.
When departments must purchase their own monitoring equipment – and pay to replace it out of existing budgets when it breaks or goes missing – their care teams may feel possessive. By moving patient monitoring costs to the site level (or even enterprise level), health systems can change how individual teams view equipment. It then belongs to the larger operation and, in a sense, to its patients.
At a basic level, removing the need to search for monitoring equipment can help address some of the stress and time demands floor teams experience. But a reliable supply of shared equipment can have other benefits, too, including enabling innovative, cross-unit workflows. To encourage a cultural shift, help teams understand how it can support their workloads and their patients, while seeking their input about how best to implement changes.
When equipment travels with a patient to different care area, the sending team needs to know they’re going to get it back in timely and appropriate fashion without having to wander the halls – if not the same set, then the equivalent. That expectation demands an organized way to return equipment, so it doesn’t just end up in nooks and crannies. Health systems have tried various strategies in response:
Regardless of the return model pursued, care teams need a way to touch base about equipment that moves between units. Possibilities include a channel on Microsoft Teams or using tasks in the EMR to make requests or flag available equipment that needs to go to the agreed-upon destination.
With old habits hard to break, accountability is paramount, as is leadership support – both in the short term and the long run. Inevitably, hiccups will emerge and troubleshooting needs arise. Ideally, the initiative should have C-suite backing, especially from the chief nursing officer, who can designate a change management leader. From there, key support comes from nurse managers responsible for process management at each unit, to help train teams and ensure equipment is shared and returned. Floor observation remains helpful, too, to check equipment flow and known stockpiling spots. Lapses provide an education opportunity – and a note to supervisors, should slips continue.
For successful adoption, training shouldn’t end once initial efforts are complete. A culture of sharing often feels novel, so requires ongoing education. Super-users can continue to support the effort, and project leaders can use huddles to provide updates, share reminders and assess progress. Reaching all care teams is critical, as a well-functioning effort to share and return equipment rests on full participation.
Such a significant change in culture and processes requires appropriate planning and thoughtful implementation. There’s a danger, though, of taking a piecemeal approach and moving too slowly. Care sites won’t benefit from having two different, and competing, systems running simultaneously. They also don’t want teams to quickly fall back into old ways. Therefore, once preparations are set, it’s time to make a full transition. The ultimate goal? Team members asking, "Haven’t we always done it this way?"
