Because every image counts
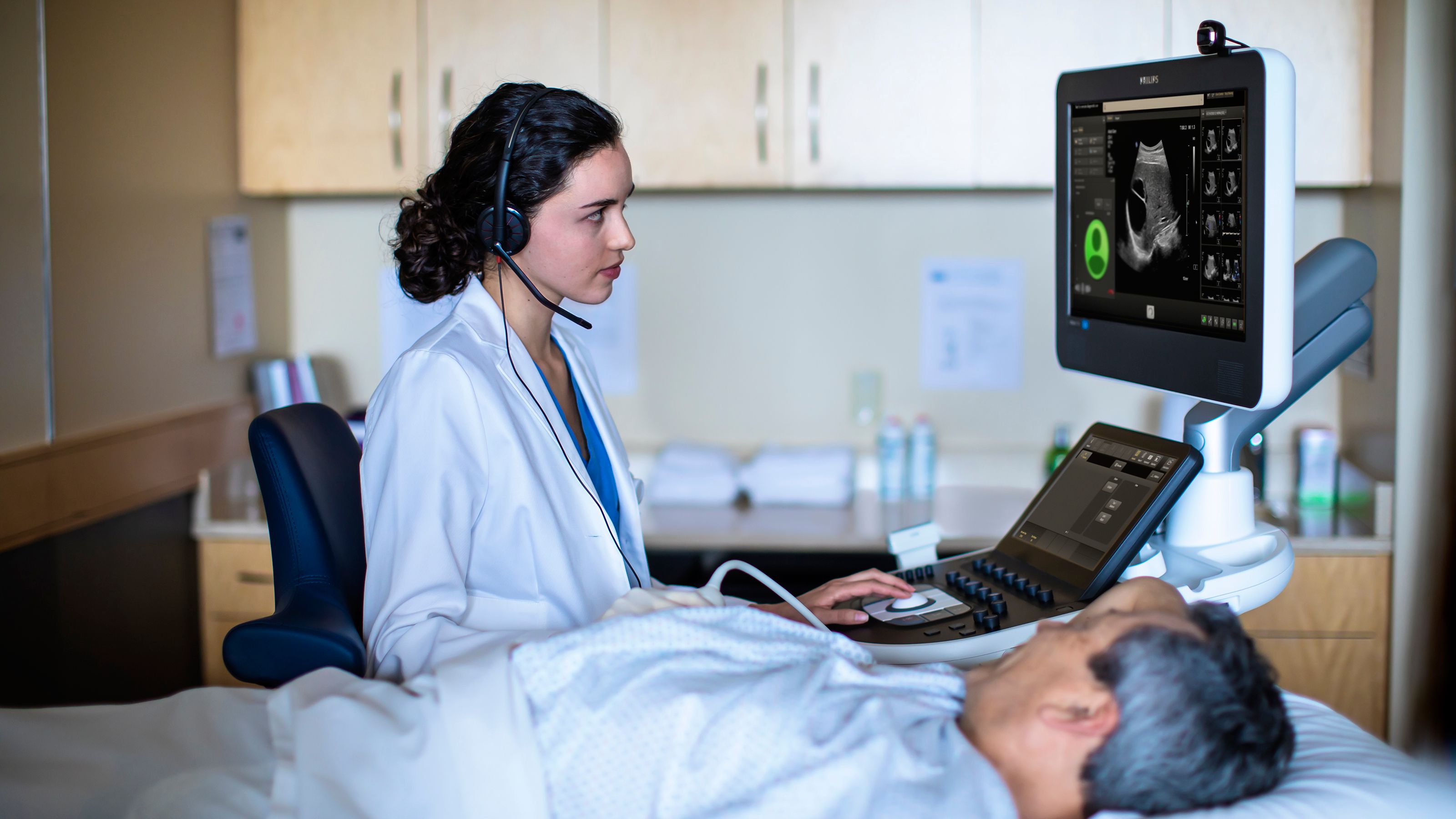
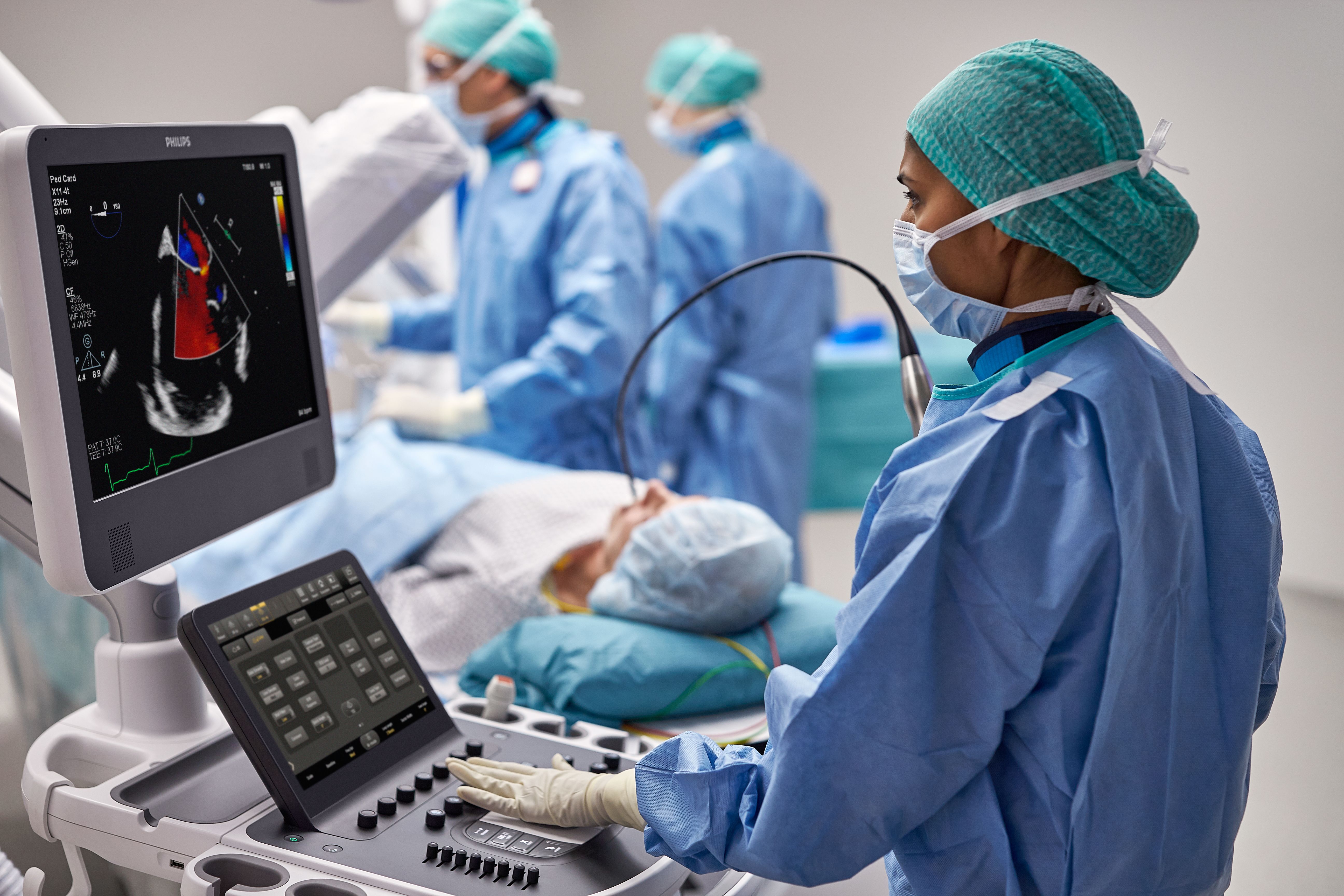
Philips ultrasound solutions connect technology, clinicians and patients to empower patient-focused care and elevate the healthcare experience. Our comprehensive portfolio – ranging from ultra-mobile handheld devices to premium cart-based systems – is designed to empower clinical confidence, with innovations that enhance imaging accuracy and performance. We’re committed to designing sustainable solutions for reliability, scalability and ease-of-use. Paired with shared architecture and comprehensive service programs, our solutions deliver lifetime value to you and your patients.

The new Flash Ultrasound System 5100 POC - built for the way you work at the point of care