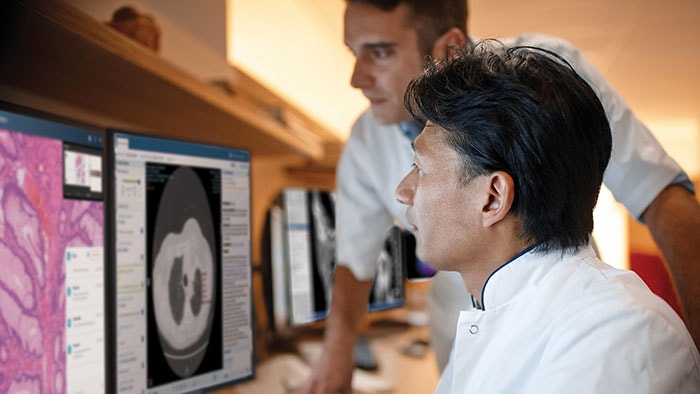
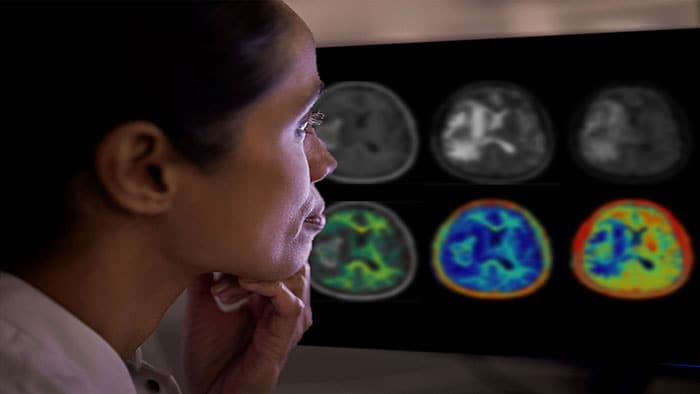
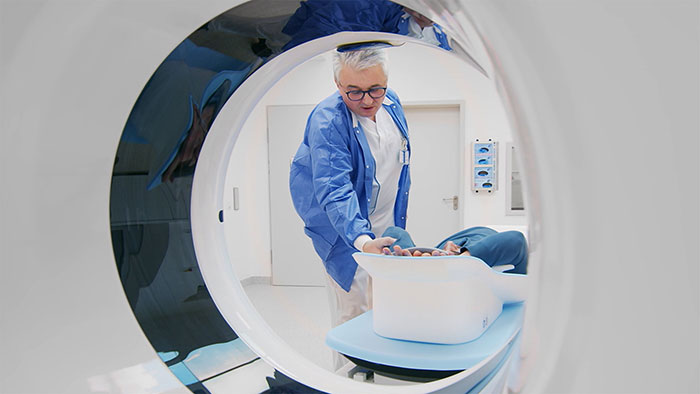
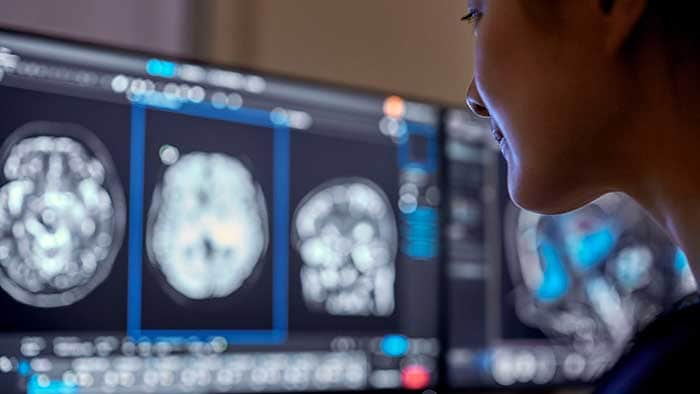
You’ve just returned from the ACC.19 in New Orleans. What were the main themes at the event? BvM: There’s always a lot going on in cardiology, but the things that stood out for me at ACC.19 were the growing interest in the use of Artificial Intelligence (AI) in cardiac care, together with important study results in the area of population health management and, of course, new developments in image-guided minimally-invasive heart valve replacement. AI is really beginning to find traction, not just in radiology but also in other clinical areas. During ACC.19’s ‘Future Hub’ session, several entrepreneurs came up with exciting future possibilities for AI in cardiology. Several important study results were also announced at the event, including the results of a large-scale study on the use of consumer wearables to identify atrial fibrillation, and the potentially game-changing results of two clinical trials on the benefits and effectiveness of minimally-invasive transcatheter aortic valve replacement (TAVR) in younger healthier patients compared to open heart surgery. Those last results were particularly interesting for us, because Philips’ interventional imaging systems and navigation software helped to pioneer and grow TAVR procedures. What did Philips showcase at ACC.19? BvM: We showcased several new developments that demonstrate our ability to accelerate the pace of innovation, including our recently introduced Azurion with FlexArm system, which sets a new standard for patient imaging and positioning flexibility for image-guided procedures, and our SyncVision iFR co-registration technology, which allows physicians to identify and optimally treat the parts of a blood vessel causing ischemia. We also showcased IntelliSpace Cardiovascular 4.1, our next-generation cardiovascular image and information management system, and our EPIQ CVx cardiology ultrasound system, which helps to increase diagnostic confidence and simplify clinician workflows in cardiac care. Plus, we highlighted the results of the DEFINE-PCI study, which assessed the level of residual ischemia in patients after percutaneous coronary interventions (PCIs). What is the significance of the DEFINE-PCI study results? BvM: This 500-patient, multicenter, blinded physiologic assessment study used Philips’ iFR pullback measurement technology to understand the rates and causes of residual ischemia (reduced blood flow) after a stent is placed. The study found that nearly one in four patients had residual ischemia after coronary stent implantation aimed at relieving severe blockages. In most cases, this was due to an untreated blockage not identified using X-ray angiography alone. Physiologic guidance tools such as Philips’ SyncVision iFR co-registration offer a simple solution for the detection of such blockages that integrates into existing workflows. It’s a great example of how Philips is combining image guidance, devices and smart intuitive software to deliver better cardiac care and improved patient outcomes.
Philips’ SyncVision iFR co-registration is a great example of how we are combining image guidance, devices and smart intuitive software to deliver better cardiac care and improved patient outcomes.
What is Philips doing in Artificial Intelligence? BvM: At Philips, we prefer to talk about adaptive intelligence rather than artificial intelligence, reflecting our belief that AI needs to be contextualized and applied in a meaningful way that improves people’s lives, whether they are physicians, patients or healthy individuals, by adapting to their needs and extending their capabilities. Take our IntelliSpace Portal visual analysis software for example, which uses machine learning to improve clinician workflows. We’re also taking the output from our patient monitoring systems and applying adaptive intelligence to predict which patients are likely to get worse in the coming hours. Developments like these are only the start. Today, around one in every two of Philips’ R&D professionals is active in software and data science, and for many of them AI is increasingly becoming a daily part of their lives. Meanwhile, there is also much attention being given to the treatment of peripheral vascular disease with paclitaxel-based drug-coated balloons and drug eluting stents. The FDA has recently sent a follow-up letter to healthcare providers with their preliminary analysis and recommendations. What is your view on this? BvM: Firstly, please let me stress that patient safety is our top priority. In that respect, it is important to note that since there is no 5-year follow-up data yet from the pivotal premarket randomized clinical trial for our Stellarex drug coated balloon, the Stellarex trial was not one of the three trials with data referenced by the FDA, which showed a signal of increased long-term mortality. Moreover, at three years, follow-up data from the Stellarex trial do not show any such signal.
Stellarex is unlike any other drug-coated balloon in the industry for the treatment of peripheral artery disease. Stellarex has a unique low drug dose and drug coating composition, and we have dedicated clinical studies with three-year follow-up data that demonstrate the safety and efficacy of Stellarex.
It is also important to note that Stellarex is unlike any other drug-coated balloon in the industry for the treatment of peripheral artery disease. Stellarex has a unique low drug dose and drug coating composition, and we have dedicated clinical studies with three-year follow-up data that demonstrate the safety and efficacy of Stellarex in restoring and maintaining blood flow to arteries in the legs of patients with peripheral artery disease. Stellarex delivers top-tier outcomes with the lowest therapeutic drug dose in common to complex patients, and has a strong safety profile. This was reinforced by a recent independent, third party, pooled analysis of patient-level data on over 2,300 patients treated with Stellarex, which demonstrated low mortality rates through three years after the treatment with no device-related deaths as adjudicated by independent Clinical Events Committees (CECs). We are confident in our data and the safety profile of our unique low-dose Stellarex drug-coated balloon. Bert van Meurs is Executive Vice President and Chief Business Leader of Image-Guided Therapy, and a member of the Royal Philips Executive Committee. Bert has more than 30 years of experience in various leadership positions in research & development, clinical science and marketing & sales in Europe and Asia.