How hospitals are adapting in the face of COVID-19
As COVID-19 has swept across the globe, healthcare organizations and frontline workers have evolved their response to the pandemic as new information, opportunities and support become available. With care providers worldwide adapting quickly in recent months, COVID-19 has proven to be a catalyst for healthcare transformation. On Tuesday, July 21, Philips’ Chief Medical Officer, Jan Kimpen, and Head of the Medical Office for Connected Care, Huiling Zhang, led a discussion with five healthcare leaders and frontline clinicians on “Anticipating the new normal: How hospitals are adapting in the face of COVID-19.” Sharing learnings from managing the first wave of COVID-19 patients and plans to handle the sustained challenges, the event featured insights from: The pandemic’s tsunami effect across the globe has meant each health system has faced their own unique challenges with patient populations at different times, but several consistent themes have emerged:
Learning and adapting in unprecedented times
COVID-19 is a heterogenous disease. Presenting symptoms – especially related to respiratory failure – have varied widely. Patient populations have been inconsistently impacted, with pediatrics having significantly lower cases than the rest of the population. While they have been following guidelines for best practices, care providers have had to learn at the bedside, adapting as new information and data about patient outcomes and staff risk come to light. One example of the learning is how to manage respiratory failures of COVID-19 patients. As clinicians gain more experience, they are now more willing to use high-flow oxygen support and non-invasive ventilation approach before engaging intubation and invasive ventilations.
Technology enabling health systems to maximize capacity and resources
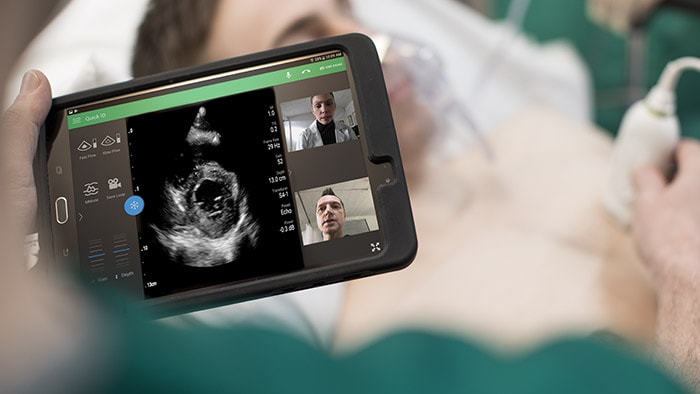
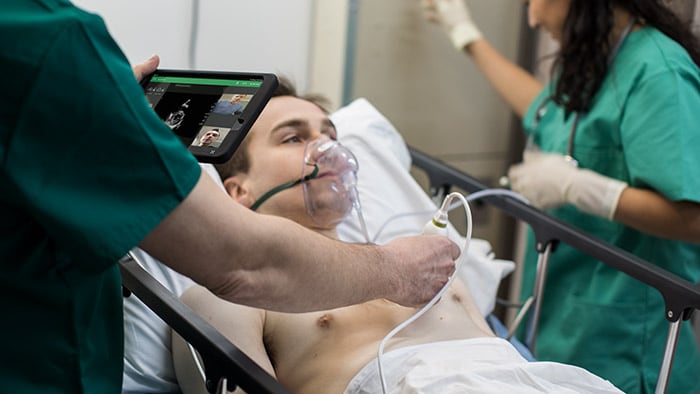
The unprecedented burden on health systems led to strains on all resources, including intensive care unit (ICU) beds, availability of appropriate staff, and access to adequate personal protective equipment (PPE). Technology such as tele-critical care and operational dashboards have enabled health systems to augment bedside teams. Such resources allow health systems to load-balance with telehealth services when there is a surge in one part of the system or relocate patients to where there is open capacity. Virtualized care models also help to reduce the workload for front-line physicians by shifting ownership of activities to other providers, such as having the pharmacy work done directly with virtual intensivists. Additionally, use of tablets help bridge communication gaps between the patient and their families, as well as with the care teams, which reduces clinician exposure and PPE burn. Because of the limitations of test supplies, health systems had to make daily decisions on which populations should have priority for being tested. By building these criteria into the electronic health record (EHR) on a daily basis, clinicians have regular access to the most recent guidelines, aiding their quick decision-making. Similarly, as concerns arose around availability of other resources such as medications, embedded insights in the EHR on which patients should be prioritized have created easy-to-follow standards of care.
Clinical care staff are the most valuable resource
COVID-19 has required selflessness and sacrifice from our healthcare heroes. They have been pushed to their physical and emotional limits during this pandemic. In many situations, care providers, particularly those with ICU training, have been shifted around the hospital to meet patient demand. While technology aims to help manage their workloads and mental burden, the well-being of care providers must be managed as well. Having efficient shift schedules and trained psychologists easily accessible at any time during their shift can provide a safe and understanding outlet in times of intense surge and risk of burnout.
Rethinking everyday care empowers patients
Although the fear of catching COVID-19 caused many patients to defer in-person care, technology has empowered patients to become more involved in their own health in new ways. Patient portals have become tools of engagement, and telehealth via video visits and asynchronous consults has increased exponentially in outpatient settings. As the shift to in-person care returns, new processes will enhance the patient experience, such as virtual check-ins that allow patients to wait safely in their cars until their appointment time.
The new normal requires a continued shift in mindset
There will be a long road to recovery, but there are several steps the healthcare industry must take in this journey: The webcast on “Anticipating the new normal: How hospitals are adapting in the face of COVID-19” is now available to listen in its entirety.

Share on social media
Topics
Contact

Kathy O'Reilly
Philips Global Press Office Tel.: +1 978-221-8919
You are about to visit a Philips global content page
Continue