How digital innovation can bring healthcare to remote regions: three real-world examples
Apr 02, 2021 - Reading time 7-9 minutes
Accessing timely and specialized health services can be a challenge for patients living in remote or rural communities. But thanks to innovative technologies and local care networks, patients in both developing and developed countries can get the healthcare they need closer to home. Bringing care directly to communities and into the homes of patients helps address disparities in healthcare that often impact our nation’s, and the world’s most vulnerable populations. Philips aims to extend care wherever it’s needed, with the goal of improving the lives of 2.5 billion people a year by 2030.

Offering easier access to healthcare in rural areas of the US
In some rural areas of the United States, patients must travel hours to access care, particularly when they need specialized diagnostic and treatment services for complex diseases. Innovative telehealth technology can ease this burden for rural patients. Remote patient monitoring devices and sensors, for example, are convenient options for clinicians to track patients’ vital signs and manage chronic conditions within the home.
Some patients, however, do not have the necessary digital devices, reliable household internet, or the privacy needed for sensitive clinical conversations at home. An option that offers patients a community-based choice for remote care is the Virtual Care Station. This telehealth environment has been developed by Philips to provide virtual face-to-face care in convenient neighborhood locations such as retail settings, libraries, universities, and veteran service organizations.
Virtual Care Stations are connected to regional medical centers and equipped with specialized staff and technology. Each Virtual Care Station features enough room to accommodate a patient in a wheelchair or with an accompanying care partner or service animal.

Virtual Care Stations are designed to deliver an enhanced telehealth experience in a convenient location.
The Virtual Care Station is based on technology developed for the US Department of Veterans Affairs’ (VA) telehealth program (ATLAS). The VA delivers healthcare services to nearly 9 million veterans, many of whom live in remote locations and are coping with one or more significant chronic conditions like diabetes, heart disease and depression. The VA offers a range of remote access solutions, including at-home virtual care, real-time video access to specialists from community clinics, and their Tele-ICU program that brings specialty providers into the local intensive care unit room.
These telehealth innovations give providers new access to patients, allowing doctors to virtually diagnose and manage patient care. The biggest win is improving the veteran care experience, allowing patients to avoid unnecessary hospital stays and lengthy travel to see providers and remain independent at home.
Partnerships like this one are essential for ensuring the highest quality care reaches rural populations and underserved communities in the US. In 2021, Philips is partnering with Navajo Nation to set up a point-of-care ultrasound (POCUS) solution training program, which will equip Navajo clinicians with the tools and knowledge to provide remote and portable ultrasound capabilities for their communities.
Bringing maternal care to remote communities in Africa
In remote African communities, there is often an acute shortage of trained ultrasound specialists. Pregnant women living in the vast rural areas of Kenya, for example, may have to travel many hours to the nearest hospital. This makes it difficult for these women to adhere to the World Health Organization’s recommendation that every pregnant woman should undergo at least one ultrasound scan, preferably in the first 24 weeks of pregnancy, to accurately estimate gestational age, detect fetal anomalies, and improve a woman’s overall pregnancy experience.
That’s why the Philips Foundation, together with local clinical partners and the Ministry of Health, is working to put portable ultrasound into the hands of trained midwives at primary care facilities and connect these midwives to specialists in urban hospitals. Through a combination of in-person training, remote education, and real-time video collaboration, midwives can build the skills and confidence required to perform routine basic obstetric screenings. They can identify high-risk women for timely referral and treatment and give these pregnant women a much better chance of bringing a healthy child into the world.
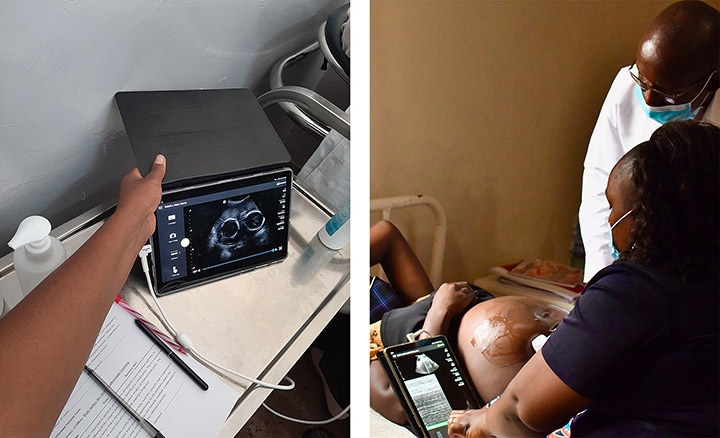
Midwives at rural health clinics in Kenya can now conduct basic ultrasound exams on pregnant women and share data remotely for virtual collaboration (Photos: Amref Health Africa)
Midwives can also build health profiles of pregnant women in a simple mobile app by collecting data from physical exams at primary care facilities or even at the soon-to-be-mom’s home. This data generates a risk score that can help caregivers identify who may need extra care. For expecting moms, an educational app delivers pregnancy-related tips and allows them to track pregnancy symptoms, kick count, and medication usage. Moms can then share that data with caregivers.
With the right remote support, trained midwives in primary care facilities can play an integral role in early detection, diagnosis, and follow-up of pregnancy and pregnancy-related complications. Patient data can be shared digitally across locations, enabling virtual consultation, remote diagnostic assistance and monitoring. Overall, this helps create a more connected maternal care ecosystem in which pregnant moms in remote locations have better access to the care they need.
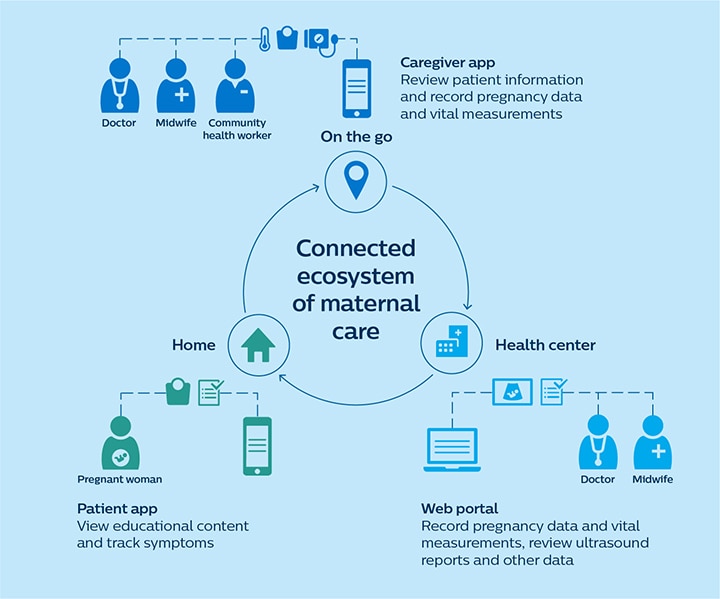
A digital maternal care ecosystem allows doctors, midwives, and community healthcare workers to share patient data, including lab tests and ultrasound data.
Bringing image-guided therapy to rural communities in China
The geographical divides that make healthcare access a challenge in rural parts of the US and Kenya also exist in China. Like other countries, China’s medical institutions and highly qualified healthcare providers have historically concentrated in cities. These metropolitan hospitals are typically equipped with state-of-the-art medical systems and devices, unlike rural areas where specialized staff and equipment tend to be in short supply.
For patients in remote areas who experience sudden heart attack or stroke, accessing treatment may mean travelling hours to reach the nearest big-city hospital where clinicians can perform image-guided, minimally invasive procedures. This access barrier can severely decrease the chances of timely care and survival.

Local treatment centers bring lifesaving care closer to rural patients.
Fortunately, progress is being made in China to close the gap between urban and rural healthcare services. For example, Philips is collaborating with county-level hospitals to set up local treatment centers for patients with chest pain or stroke. These centers take an integrated approach that covers the entire care pathway: from early diagnosis of a patient’s condition in the ambulance and further diagnostic tests in the hospital, to minimally invasive procedures in the cath lab and patient monitoring in the ICU.
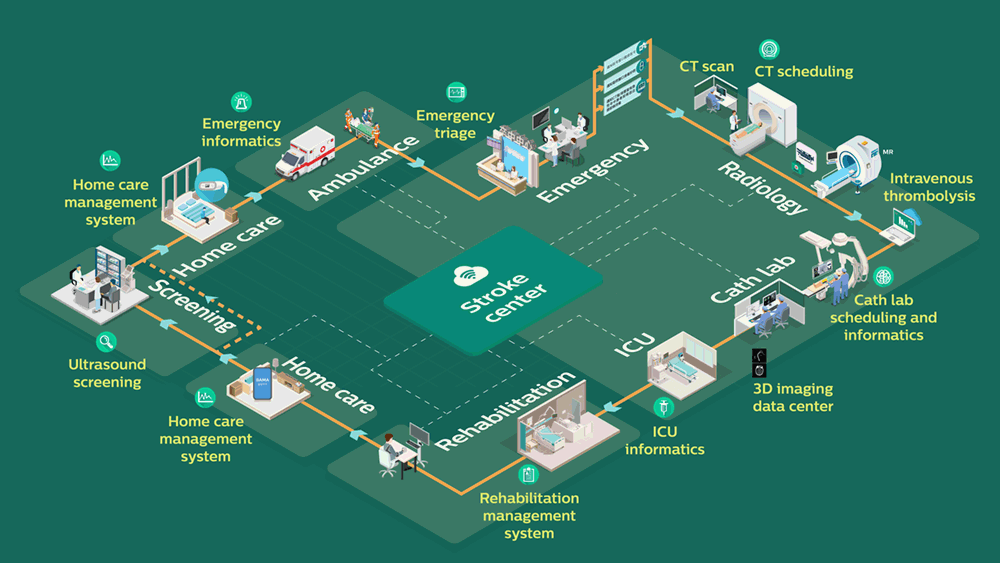
The Stroke Center in operation: integrated patient pathway from diagnosis to minimally invasive treatment and aftercare.
Supported by seamless data exchange across settings, this connected approach helps get patients to appropriate and effective treatment as soon as possible, followed by the right after-care. The centers bring lifesaving healthcare closer to rural patients and help patients recover faster and have better treatment experiences.
Shared commitment to improving healthcare access
These are just three examples that illustrate how healthcare providers can leverage digital technology and local, network-based facilities to increase access to healthcare for people living in rural areas around the world. New innovations are being developed every day, and Philips continues to pioneer digital health technologies, partnering with local providers to improve access to quality healthcare, no matter where people live.
Click here to learn about how we can work together to help transform patient care and further innovation, regardless of location.








